These are consequences of sleeping with…
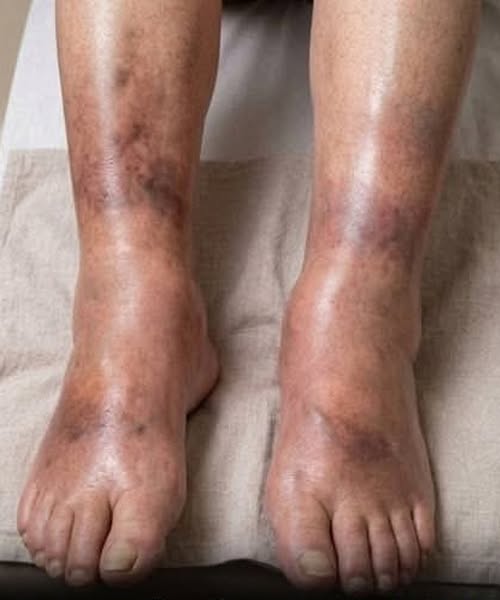
The silent signal: What your swollen legs may reveal about pancreatic can:cer
It is not uncommon for the human body to reveal internal distress through symptoms that appear unrelated to the original source of illness. Many serious diseases, including cancers, often begin quietly and produce only mild signs before more noticeable symptoms emerge.
The pancreas, located in the abdominal cavity behind the stomach, plays a crucial role in digestion and regulating blood sugar levels. Due to its deep position in the body, pancreatic disorders frequently advance without clear symptoms during their early stages. This is why pancreatic cancer, in particular, is often discovered only after it has already progressed.
Recent scientific research suggests that the body may sometimes reveal early warnings of disease in unexpected ways. One such potential sign is swelling in the lower limbs. Swollen legs, also known as edema, are commonly associated with kidney disease, heart conditions, or poor circulation.
However, newer clinical studies indicate that leg swelling may also signal more serious health problems, including pancreatic cancer, according to research published in the National Library of Medicine. Although edema itself is relatively common, the circumstances surrounding its appearance can provide important clues to the underlying cause. Sudden swelling, swelling that is more severe in one leg than the other, or persistent swelling without an obvious reason may point to deeper systemic changes occurring inside the body.
Today, researchers understand that pancreatic cancer can alter blood chemistry, circulation patterns, and protein levels in the bloodstream—changes that may sometimes manifest through symptoms in the legs.
Recognizing such warning signs may contribute to earlier detection of the disease.
The Primary Culprit: Deep Vein Thrombosis (DVT)
The strongest and most concerning connection between swollen legs and pancreatic cancer is the formation of blood clots, particularly a condition known as Deep Vein Thrombosis (DVT). This occurs when a clot develops deep within a vein—most often in the leg—blocking normal blood flow. According to the Mayo Clinic, symptoms can include swelling, warmth, pain, and sometimes a change in skin color in the affected limb.
Among various cancers, one stands out for its particularly strong association with these clots: pancreatic ductal adenocarcinoma (PDAC). This cancer has such a powerful link with clot formation that physicians often describe it as “procoagulant,” meaning it actively promotes the thickening and clotting of blood far more rapidly than normal.
This effect is not simply a side consequence of illness but a direct biological result of how the cancer interacts with the body’s systems.
The Biochemistry of Trousseau’s Sign
For many years, doctors have recognized that unexplained blood clots can sometimes signal hidden cancers. In the 19th century, a French physician named Armand Trousseau observed that several patients experienced recurring clots long before their underlying cancers were diagnosed. This medical phenomenon later became known as Trousseau syndrome.
Modern research has since clarified the mechanisms behind this relationship. Advances in molecular biology have identified several biological “triggers” used by pancreatic tumors that interfere with the body’s clotting system.
Tissue Factor (TF) Overexpression
Pancreatic tumor cells release large amounts of a protein called Tissue Factor into the bloodstream. This protein functions as the body’s primary “emergency trigger” for blood clotting, initiating the coagulation cascade—the complex sequence of reactions that ultimately forms a clot.
In addition, cancer cells shed microscopic particles containing Tissue Factor into circulation. These particles travel throughout the bloodstream, spreading clot-promoting signals to distant areas of the body. They frequently lodge in the legs, where clot formation often occurs.
Adenocarcinoma Mucins
Another important contributor involves mucins—large, sugar-coated proteins produced by many pancreatic tumors. When these mucins enter the bloodstream, they behave like adhesive bridges, attaching to platelets and white blood cells. This interaction activates them in ways that strongly encourage clot formation, as described in research published in the Journal of Mind and Medical Science.
Together, these mechanisms create what physicians sometimes refer to as “sticky blood”—a condition in which the body’s natural clotting system remains continuously activated, making it far more likely for dangerous blockages to form.
Why the Legs Are Affected
According to research published in the National Library of Medicine, blood naturally moves more slowly through the deep veins of the legs than in many other parts of the body. This happens because gravity works against the upward flow of blood and because the legs are located far from the heart. As a result, this region is particularly vulnerable to the development of blood clots.
When abnormal clotting signals circulate throughout the body, the legs are one of the most frequent locations where a blockage can develop. As a clot begins to form, it disrupts normal blood flow and quickly leads to swelling and inflammation in the affected area. Some individuals may also notice pain, warmth, or redness, but for many patients the only visible warning sign is swelling in the leg.
Statistical Risks: The Khorana Score
Clinical evidence consistently confirms a strong relationship between pancreatic cancer and disorders involving blood clots. Among all cancers, pancreatic cancer ranks second for the risk of developing venous thromboembolism (VTE), a condition that includes both deep vein thrombosis (DVT) and pulmonary embolism.
Recent estimates from 2024 and 2025 suggest that roughly 20% to 40% of people with advanced pancreatic cancer will experience a clotting event at some point during the course of their illness. This makes clotting disorders one of the most frequent complications associated with the disease.
The Khorana Risk Score
To determine which cancer patients face the highest likelihood of developing blood clots, clinicians often rely on a predictive tool known as the Khorana Risk Score. This model assesses several factors, including the type of cancer involved, platelet levels, hemoglobin concentration, and body mass index.
Each cancer type is assigned a baseline score based on its known risk of causing clotting problems. Pancreatic cancer automatically receives two points, placing patients directly into the high-risk category even before other risk factors are taken into account.
Prognostic Significance
For individuals with pancreatic cancer, blood clots are not merely a complication of the disease—they may also provide insight into how severe the cancer is. Research connected to the COMPASS trial in 2025 suggests that the early appearance of clots may be linked to particularly aggressive tumor subtypes.
When venous thromboembolism occurs within the first three months after diagnosis, it is often associated with tumors that have biological characteristics promoting faster growth and poorer survival outcomes. Because of this connection, doctors view sudden or unexplained leg swelling as a possible warning sign that the disease may progress more aggressively.
Protein Deficiencies and Systemic Edema
Not all swelling associated with pancreatic disease is caused by blood clots. In certain cases, swelling may appear in both legs due to a condition called systemic edema, which occurs when the body’s fluid balance becomes disrupted, according to the Mayo Clinic.
Albumin, a protein produced by the liver, plays a key role in keeping fluid contained within the blood vessels. When albumin levels drop too low, fluid begins to leak out of the vessels and accumulate in surrounding tissues, resulting in swelling.
Pancreatic tumors can interfere with this process because they may block the release of important digestive enzymes. Without these enzymes, the body struggles to properly absorb proteins from food. Over time, this can lead to a condition known as hypoalbuminemia, particularly in more advanced stages of the disease. In some cases, the tumor may also affect liver function or trigger widespread inflammation in the body, both of which can further reduce albumin levels.
This type of swelling commonly appears as pitting edema, which is usually most noticeable around the ankles and feet. A simple way to check for pitting edema is by gently pressing a finger into the swollen area—if a temporary indentation remains, it may indicate this condition. Unlike swelling caused by DVT, which typically affects only one leg, systemic edema usually develops gradually and tends to involve both legs.
Diagnostic Pathways: When Swelling Leads to Discovery
In some cases, swelling in the legs may be the earliest sign that leads to the discovery of pancreatic cancer. Because of this possibility, medical guidelines—such as those released by ESMO in 2025—recommend careful medical evaluation when leg swelling appears without a clear explanation. This recommendation is particularly important for individuals over the age of 50 or those with additional risk factors, including a history of smoking or unexplained weight loss.
The diagnostic process for possible pancreatic disease usually begins with initial testing. Doctors often start with a blood test that measures D-dimer levels, proteins that appear when the body is breaking down a blood clot. Research published by Seitz and colleagues in 2024 showed that elevated D-dimer levels can indicate the presence of a clot, although the test alone cannot confirm a diagnosis.
If deep vein thrombosis (DVT) is suspected, physicians typically proceed with imaging tests. According to the Mayo Clinic, one of the first methods used is duplex ultrasound, which allows doctors to observe blood flow in the veins and determine whether it has slowed or become blocked.
Another important step involves identifying any underlying cancers. When DVT occurs without an obvious trigger—such as recent surgery or long-distance travel—it is considered unprovoked. In such situations, the National Cancer Institute noted in 2025 that physicians may order abdominal CT or MRI scans to search for hidden cancers, including pancreatic cancer. Investigating unexplained clotting events can sometimes lead to the detection of cancer at an earlier stage than would normally occur.
Management and Emerging Treatment Strategies (2025–2026)
When leg swelling is linked to pancreatic cancer, treatment focuses both on relieving the swelling and addressing the underlying cause.
Anticoagulation Therapy
Once a blood clot is identified, doctors commonly prescribe anticoagulant medications such as Direct Oral Anticoagulants (DOACs) or Low-Molecular-Weight Heparins (LMWH). These medications help prevent the clot from enlarging and reduce the risk of new clots forming. They also significantly lower the chance of severe complications, including pulmonary embolism.
Preventive Strategies
Recent findings reported in the ASCO Post suggest that patients considered at high risk may benefit from preventive use of blood-thinning medications at the time of their cancer diagnosis in order to reduce the likelihood of clot formation.
Supportive Care
In addition to medical treatment, certain practical measures can help relieve symptoms and reduce fluid buildup. According to the Mayo Clinic, helpful steps include:
Wearing compression stockings to improve circulation
Elevating the legs while resting
Staying physically active through light exercise such as walking
